 In 2014, parents Pam and Chris Andrews noticed their oldest daughter Belle was showing some developmental delays in her gross and fine motor skills. Because she was only 3 years old and the delays were subtle, it was hard to know what was normal development and what was cause for concern. But Pam and Chris sensed something was wrong. Over several years, they sought answers from a multitude of specialists, including speech, vision, and physical therapists, neurologists, oncologists, ENTs, nephrologists, and endocrinologists. Their search culminated when Drs. Amy White and Mary Elizabeth Parker advised them to have Belle’s genome analyzed by Whole Exome Sequencing to look for potential genetic diseases.
In 2014, parents Pam and Chris Andrews noticed their oldest daughter Belle was showing some developmental delays in her gross and fine motor skills. Because she was only 3 years old and the delays were subtle, it was hard to know what was normal development and what was cause for concern. But Pam and Chris sensed something was wrong. Over several years, they sought answers from a multitude of specialists, including speech, vision, and physical therapists, neurologists, oncologists, ENTs, nephrologists, and endocrinologists. Their search culminated when Drs. Amy White and Mary Elizabeth Parker advised them to have Belle’s genome analyzed by Whole Exome Sequencing to look for potential genetic diseases.
 Test results revealed that Belle, then 5 years old, had Niemann-Pick Disease Type C (NPC), a genetic disease so rare that Pam and Chris had never heard of it. The incidence of NPC is estimated to be about one case per 100,000 live births. There are currently about 2,000 diagnosed cases of NPC worldwide.
Test results revealed that Belle, then 5 years old, had Niemann-Pick Disease Type C (NPC), a genetic disease so rare that Pam and Chris had never heard of it. The incidence of NPC is estimated to be about one case per 100,000 live births. There are currently about 2,000 diagnosed cases of NPC worldwide.
Shortly after receiving Belle’s results, the Andrews’ geneticist Dr. James Gibson suggested testing Abby, their 2-year-old daughter. The family’s pain more than doubled when Dr. Gibson confirmed Abby also had NPC.
NPC is an ultra-rare, progressive, and fatal neurovisceral disorder with highly heterogeneous symptoms that cause progressive deterioration of the central nervous system. Caused by mutations in the NPC gene, the disease can be inherited if both parents carry the mutation in the same NPC gene. A very rare occurrence.
After pouring over the research and talking with other NPC families, the Andrews family found some solace in a small community of NPC families who were able to share their journey. They also learned of a clinical trial being conducted to evaluate a drug called VTS-270 for treating NPC. There is currently no FDA-approved drug to cure or slow the progression of NPC.
 Through tireless efforts by Pam and Chris, Belle was enrolled into the clinical trial and Abby was granted compassionate use of the drug. With very few hospitals in the United States participating in the clinical trial, the Andrews family had to travel to Chicago every two weeks so the girls could receive treatment. This obviously took an emotional, physical, and financial toll.
Through tireless efforts by Pam and Chris, Belle was enrolled into the clinical trial and Abby was granted compassionate use of the drug. With very few hospitals in the United States participating in the clinical trial, the Andrews family had to travel to Chicago every two weeks so the girls could receive treatment. This obviously took an emotional, physical, and financial toll.
With long family ties in Austin, the Andrews reached out to everyone they knew who might have connections with Dell Children’s Hospital, a local research hospital they believed would be a prime candidate for participating in the VTS-270 trial. Through their vigilant efforts, Dell Children’s heeded the call of these vulnerable children and became a site where any affected child in their region could receive participate in the trial.In October of 2017, just seven months after their NPC diagnoses, Belle and Abby began receiving the investigational therapy VTS-270 at Dell Children’s Hospital, a 10-minute drive from home. On therapy since before visible signs and symptoms began, Abby is showing some developmental delays, which according to NPC experts, are a sign of disease progression in young children. Despite losing the ability to walk without assistance, Belle remains stable since she began treatment. In fact, she has gotten a bit better in some daily activities such as swallowing.
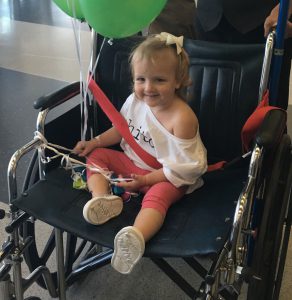 The Andrews family continues to hope the clinical trial results in FDA approval of VTS-270 which would allow their daughters and other children afflicted with NPC to have access to a therapy that has been proven to effectively and safely treat this insidious disease.
The Andrews family continues to hope the clinical trial results in FDA approval of VTS-270 which would allow their daughters and other children afflicted with NPC to have access to a therapy that has been proven to effectively and safely treat this insidious disease.